In this section:
Plantar Heel Pain Fat Pad SyndromePain Activity Ladder Ankle, Foot and Toe Exercise
Plantar Heel Pain
What is Plantar Heel Pain?
This is by far the most common condition affecting the foot; one in ten people develop it at some time in their life. It is most common in people between the ages of 40 and 60 years; however, it can occur at any age. Women are twice more likely to develop this condition than men. It is also common in athletes. The good news is that with appropriate advice and treatment this will resolve for the vast majority of people.
Treatment protocols for heel pain almost always start with basic principles and we would encourage you to consider trying some self-help treatment before making a referral to your local Podiatry department.
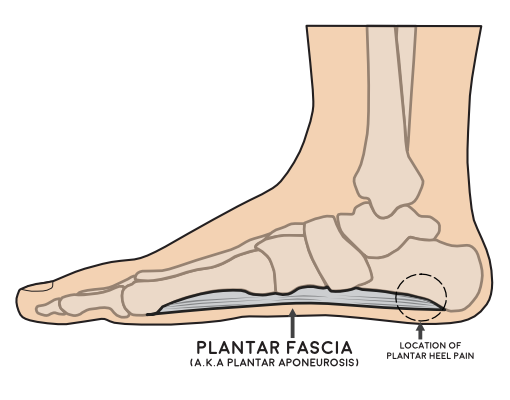
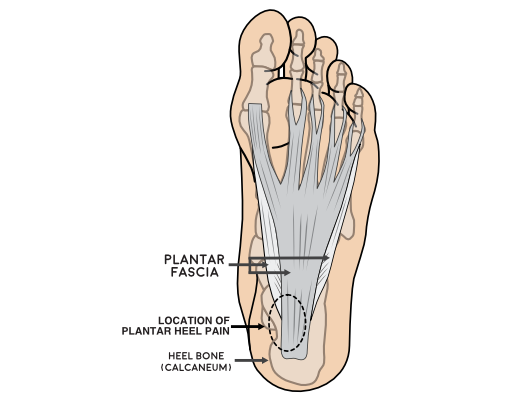
The plantar fascia is a strong fibrous band that stretches from the heel to your toes. It is made up of three bands that run along the inside, middle and outside of the bottom of your foot. The inside and outside bands support the arch and act as shock-absorbers.
Shock absorption is important as it reduces the impact your body weight has on the foot when walking, running and carrying out any weight-bearing exercises. Not only does the plantar fascia support the arch, but it also stabilizes the foot to allow you to push off through your toes.
When pain develops in the plantar fascia, it can be very disabling. Every step can become more painful and cause you to change the way that you walk. When this happens it can lead to strains to other parts of your body.
Also known plantar fasciopathy used to be called plantar fasciitis, this is the most common condition affecting the foot. The condition is usually diagnosed by clinical findings alone.
You may experience any or all of the following:
- A gradual onset of pain affecting the base of the heel
- Pain in the heel during the first steps when you get out of bed in the morning
- Pain in the heel when weight bearing after a period of inactivity or rest
- Pain that eases or lessens with moderate activity
- Worsening pain later on during the day or after long periods of standing or walking
In most cases, plantar heel pain develops as a result of changes to the way our foot functions with small tears occurring within the plantar fascia. These injuries happen at a rate faster than the body can heal them and as a result the plantar fascia starts to become thickened and painful. The pain is most commonly felt under the inside of the heel but can be anywhere along the bands of the plantar fascia.
You may have contributing factor related to plantar heel pain:
- Being overweight
- Weakness in the muscles within your feet or leg
- Tightness in the muscles up the backs of your legs
- Wearing unsupportive footwear such as shoes or sandals which have a low heel and don’t support the feet
- Spending long periods standing or walking, especially with a sudden increase in these activities
- Jobs that involve standing or walking on hard surfaces for long periods of time
- Sudden increase in physical activity levels- for example, recently started running
Unfortunately there is no quick or easy fix and your symptoms won’t improve overnight. Plantar heel pain is self-limiting and in many cases will improve without any treatment. It is important though that if you have any of the contributing factors you make the necessary changes to help your recovery.
Making changes to your lifestyle as well as reducing aggravating activities is key to helping your recovery. Only you can do this.
There are a number of things you can try including:
- Rest and raise your foot on a stool when you can
- Put an ice pack (or bag of frozen peas) in a towel on the painful area for up to 20 minutes every 2 to 3 hours
- Wear shoes with cushioned heels and good arch support
- Use insoles or heel pads in your footwear
- Try regular stretching and foot exercises
- Try exercises which put no pressure on your feet, such as swimming
- Try to lose weight if you’re overweight or obese
These a number of things to try to avoid including:
- Avoid walking or standing for long periods
- Avoid wearing high heels and tight pointy shoes
- Avoid wearing flip-flops or backless slippers
- Avoid walking barefoot on hard surfaces
Fat Pad Syndrome
What is Fat Pad Syndrome?
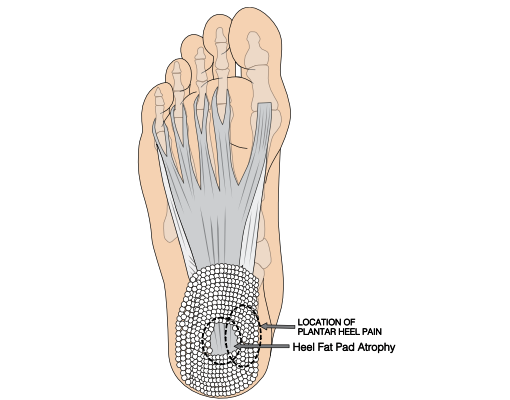
Fat pad syndrome is a condition that usually happens in the centre of your heel and is most often due to thinning and degeneration of the fat pad. Symptoms can appear very similar to those of plantar fasciopathy.
However, fat pad syndrome differs slightly. With initial first steps in the morning and after periods of rest, the discomfort is not as painful, the pain tends to build with increased weight bearing activity.
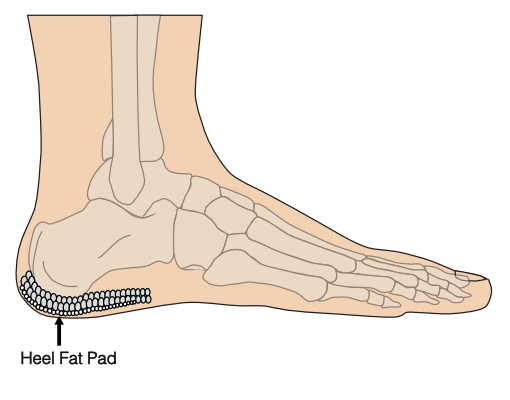
The plantar fat pad is the soft tissue layer in between the skin and the heel bone. It has a honeycombed structure with fibro-elastic chambers containing fat globules which helps with shock absorption and the spreading of pressure across the surface of your heel during activity.
Reduced shock absorption will make the heel bone more vulnerable to repetitive microtrauma. This can lead to chronic inflammation, bruising, swelling and pain within the heel bone.
Increased load can lead to irritation/ inflammation of the bursa which sits under the fat pad. A bursa is a small fluid filled sack that is found between the heel bone and the soft tissue. The bursa helps with shock absorption and to reduce friction.
In most cases, fat pad syndrome develops as a result of repeated overuse.
You may have contributing factor related to fat pad syndrome:
- Being overweight
- Age (from 30+ years) natural thinning of the fat pad
- Wearing inappropriate unsupportive footwear
- Spending long periods standing or walking, especially with a sudden increase in these activities
- Diabetes
- Inflammatory conditions i.e. rheumatoid arthritis, psoriatic arthritis etc.
- Weakness in the muscles within your feet or leg
- Tightness of the muscles in the backs of your legs
- Not allowing adequate recovery time between activities
- Prolonged use of oral corticosteroids
Unfortunately there is no quick or easy fix and your symptoms will not improve overnight. The advice below is focused on reducing your symptoms to help you get back to normal activity. Most peoples’ symptoms improve but it may take several months to get better.
Making changes to your lifestyle as well as reducing aggravating activities is key to helping your recovery. Only you can do this.
There are a number of things you can try including:
- Rest and raise your foot on a stool when you can
- Put an ice pack (or bag of frozen peas) in a towel on the painful area for up to 20 minutes every 2 to 3 hours
- Wear shoes with cushioned heels and good arch support
- Use insoles or heel pads in your footwear
- Try regular stretching and foot exercises
- Try exercises which put no pressure on your feet, such as swimming
- Try to lose weight if you’re overweight or obese
These a number of things to try to avoid including:
- Avoid walking or standing for long periods
- Avoid wearing high heels and tight pointy shoes
- Avoid wearing flip-flops or backless slippers
- Avoid walking barefoot on hard surfaces
Pain Activity Ladder
By following the pain activity ladder you can identify activities that you would consider severely painful, moderately painful and mildly irritating and act to change your habits.
The pain scale, most often used in healthcare, measures pain from 0-10 (zero being no pain and 10 representing the worst pain you could imagine).
If you can identify the level of pain you are experiencing, you will find out if you are in the green, amber or red zone. The best way to move down to the green zone is by pacing and spacing your activity.
When you are completing your rehabilitation exercises it is often best to work within the green (and sometimes amber zones depending on what you deem is an acceptable level of pain) both during the exercises and within 48 hours of completing your exercises. If you find yourself in the red zone you are likely pushing yourself too hard and may flare up the pain.
Ankle, Foot and Toe Exercise
The following exercises will help to improve your pain over a period of time. Remember to follow the advice from the Pain Activity Ladder section above.